September 2021 Newsletter
September 2021 Newsletter
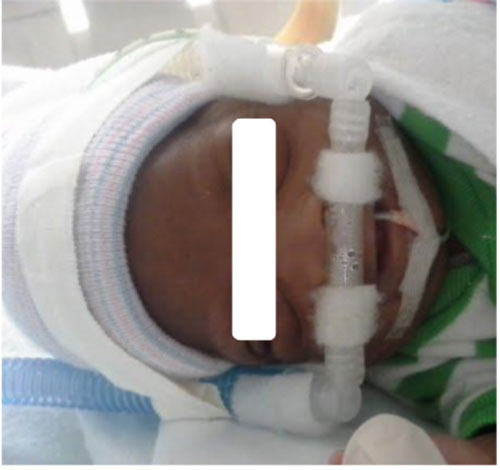
Sorry to bother you again! We just recently discussed nasal injury, how to document it, and a pathway for treatment. I saw your protocols for nasal septum protection and bedside checklist addressing these issues. My question is what to do in cases with just erythema (stage 1) just applying the anti-inflammatory and watching more carefully? What about stage 3 with full necrosis? hopefully, we won’t get this but would you consider alternatives approaches such as intubation, ENT/plastic consult, etc? Is there any specific guidelines based on the stages of wound injury?
The best approach regarding nasal septal erosion is prevention. Vigilance of bedside nursing, leaving 1-2 mm of the prongs out of the nasal aperture at all times and frequent checking are the keys.
In case nasal septal stress started to occur and you see septal redness (stage 1), you may continue using nasal prongs however, be sure you are using the right size (larger sizes cause over-stretching) and you may use anti-inflammatory or Medihoney gel (under trial).
In case of significant nasal septal erosion, you will need septal rest for 48-72 to allow healing. During which you may use nasal mask (by F&P, BabiPlus, extra). Only, if the infant is unstable or not responding to the nasal mask, you need to intubate and mechanically ventilate such infant. Keep in mind, nasal mask is not ideal for long term use. As soon as the septum heals, you need to return to using nasal prongs.
Hi – I attended the virtual conference back in December and recall mention of a 7 point checklist in The 2012 Atlas of Procedures in Neonatology. I was trying to find the checklist today and could not find it. Can you help me find this checklist?
On this website (www.bcpap.org) under the Quality page “how to start a bubble CPAP program in your unit” you will find several policies, the ‘bedside check list‘ and the monthly ‘auditing points list’ extra that you can download for free.
Hoping this help and feel free to contact us for any other questions.
We have been using bCPAP in our unit for almost 10 years and love it! I do have a couple of other questions:
- 1. In the conference, there was discussion of discontinuing bCPAP at 32 weeks and at 1200 grams. Do you recommend babies meet both criteria or is one sufficient? Our policy has been a little vague regarding this and I favor 32 weeks because it eliminates the concerns re: LGA/SGA as well as the fact that when I think about fetal lung development, I tend to think of it on a weeks of gestation basis.
- 2. Do you use any sort of topical cream for septal/columellar concerns? We have historically used Bactroban (though I don’t know how we arrived at that) but one of our neighboring institutions uses AYR Saline gel. I know the best approach is to avoid septal/columellar pressure and breakdown, of course, so we are working on that as well.
The main idea behind timing of weaning off bubble CPAP is when you think the infant’s lung has reached enough maturity. Using GA makes sense if you are sure about the dates. Weight also reflect maturity if it is healthy weight gain and not fluid overload. So, using either one as your mark to start weaning process I should eventually lead you to the same results. However, as you mentioned, it is better to agree on one of them and have a clear policy for all your team members. I will recommend using the GA.
We don’t recommend routine use of topical antibiotics or gels as they may make the prongs slippery and they may slide deep into the nostrils causing septal compression. Do you use cannulaid on top of the Velcro ad we described in the video? If you do it should be enough.