Families and the Public
• August 15, 2022
Risks and Benefits of CPAP treatment for newborns
Risks and Benefits of CPAP treatment for newborns
A CPAP machine is a common tool used in Neonatal Intensive Care Units (NICU) to help premature infants breathe. The machine forces air into the baby’s lungs, which helps them expand and prevents collapse. CPAP treatment is typically used when a baby is born before 32 weeks gestation or has a birth weight of fewer than 1500 grams. It is also used when a baby has respiratory distress syndrome (RDS), which is a common condition in premature babies. CPAP treatment is often used in the neonatal intensive care unit (NICU) to treat respiratory distress syndrome (RDS), a common condition in premature babies. RDS occurs when the baby’s lungs are not able to produce enough surfactant, a substance that helps to keep the air sacs inflated. CPAP helps to deliver oxygen to the baby’s lungs and prevents them from becoming over-inflated.Benefits of CPAP treatment for newborns
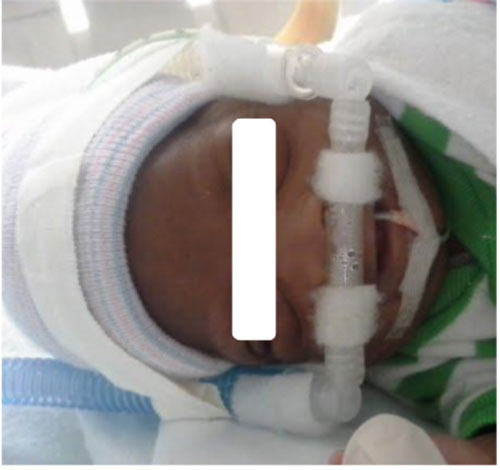
It is estimated that between 1 and 4 percent of babies are born with a condition called apnea of prematurity, in which they stop breathing for short periods of time. Apnea of prematurity often goes hand-in-hand with another condition called bradycardia, in which the baby’s heart rate slows down. While both conditions can be dangerous, they are usually benign and resolve on their own within a few weeks. However, in some cases, apnea of prematurity can lead to more serious problems, such as pneumonia, brain damage, and even death. That’s why many doctors recommend that babies with apnea or prematurity be treated with CPAP therapy. CPAP, which stands for “continuous positive airway pressure,” is a non-invasive way to keep a baby’s airway open and breathe regularly. A small, soft mask or nasal prongs is placed over the baby’s nose and mouth, and a gentle stream of air is delivered through it. The pressure from the air stream keeps the baby’s airway from collapsing and helps them to breathe more regularly. CPAP therapy has been shown to be effective in treating apnea of prematurity, and it comes with very few side effects. The most common side effect is nasal irritation, which can usually be resolved by using a different type of mask or by adjusting the settings on the CPAP machine. CPAP therapy is usually started as soon as apnea of prematurity is diagnosed, and it is typically continued for 2-4 weeks until the baby’s apnea episodes have resolved. If you are the parent of a baby with apnea or prematurity, talk to your doctor about whether CPAP therapy is right for your child.The risk of CPAP NICU for preterm infants
Preterm infants are at increased risk for a number of respiratory problems, including bronchopulmonary dysplasia (BPD), and are often treated with continuous positive airway pressure (CPAP) in the neonatal intensive care unit (NICU). However, CPAP treatment may be associated with an increased risk of adverse effects. The main complications associated with CPAP are:- Pneumothorax
- Air leaks
- Sinusitis
- Otitis media
- Gastroesophageal reflux
- Rhinitis
- Facial deformities.