FAQ
• February 2, 2023
February 2023 Newsletter
February 2023 Newsletter
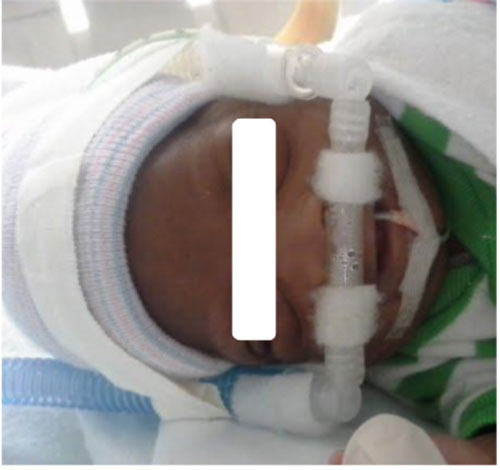
We have been using nasal prongs to deliver CPAP to our extremely low birth weight neonates, however, we have been experiencing high incidence of septal injury. Which nasal interface should we use? The answer to your question ‘which nasal interface to use with bubble CPAP’ has recently been a matter of debate. Early in the history of the evolution of bubble CPAP, only Hudson prongs were available. Currently we have several options and with the aggressive marketing techniques of the manufactures, it became a challenge for healthcare providers starting a bubble CPAP program at their units to choose for their NICU. To be able to decide on this issue, you need to consider several factors: – Outcomes: which nasal interface has been proven to be associated with best outcomes – Usability: which nasal interface is easier to use – Safety: which nasal interface is associated with least adverse effects – Costs: financial consideration in your unit and the prevailing providers in your hospital There have been quite a few publications that compared different nasal interfaces either on mannequin models or live infants. Some of these studies looked at immediate physiological changes such as changes in oxygen supplementation, physical implications such as resistance to flow and hypo-pharyngeal pressure generated, or complications such as association with nasal septal injury (1-10). None of them compared the association of the nasal interface with the primary outcome of interest which is chronic lung disease. To our knowledge, centers who have been adopting bubble CPAP for long time and achieved significant reduction in the incidence of chronic lung disease such as Columbia Presbyterian Children’s Hospital in New York, the George Washington University Hospital in Washington, DC or Cleveland Clinic children’s Hospital, Cleveland, OH, and similar institutions have been primarily using the traditional short curved nasal prongs that radiate from a transverse cylindrical tube and fit snuggly in the neonate’s nasal apertures. Although, one may claim that there are several other factors that are associated with the ultimate outcome of chronic lung disease (11), it remains a fact that centers who were able to reduce their CLD incidence to <10% in infants <1500g are those who primarily use such type of prongs as described above. So, our answer is, we are awaiting a randomized controlled trial that examine the use of a specific nasal interface with the incidence of chronic lung disease in comparison to short curved nasal prongs that snuggly fit in the neonate’s nasal apertures while standardizing other factors that lead to better outcomes such as avoid routine intubation at birth , short mechanical ventilation approach, strict control of supplemental oxygen, feeding and fluid management, and transfusion policies, reference #11). References- Bushell T, McHugh C, Meyer MP. A comparison of two nasal continuous positive airway pressure interfaces – a randomized crossover study. J Neonatal Perinatal Med. 2013;6(1):53-9. (PMID: 24246459).
- Singh N, McNally MJ, Darnall RA. Evaluating the Effect of Flow and Interface Type on Pressures Delivered With Bubble CPAP in a Simulated Model. Am J Perinatol. 2019 Jul;36(8):849-854. PMID: 30396227
- Green EA, Dawson JA, Davis PG, De Paoli AG, Roberts CT. Assessment of resistance of nasal continuous positive airway pressure interfaces. Arch Dis Child Fetal Neonatal Ed. 2019 Sep;104(5):F535-F539. PMID: 30567774
- De Paoli AG, Davis PG, Faber B, Morley CJ. Devices and pressure sources for administration of nasal continuous positive airway pressure (NCPAP) in preterm neonates. Cochrane Database Syst Rev. 2008 Jan 23;2008(1):CD002977. PMID: 18254011
- King BC, Gandhi BB, Jackson A, Katakam L, Pammi M, Suresh G. Mask versus prongs for nasal continuous positive airway pressure in preterm infants: a systematic review and meta-analysis. Neonatology. 2019;116(2):100-114.
- Bashir T, Murki S, Kiran S, Reddy VK, Oleti TP. “Nasal mask” in comparison with “nasal prongs” or “rotation of nasal mask with nasal prongs” reduce the incidence of nasal injury in preterm neonates supported on nasal continuous positive airway pressure (nCPAP): a randomized controlled trial. PLoS One. 2019;14(1):e0211476.
- Imbulana DI, Manley BJ, Dawson JA, Davis PG, Owen LS. Nasal injury in preterm infants receiving non-invasive respiratory support: a systematic review. Arch Dis Child Fetal Neonatal Ed. 2018;103(1):F29-F35.
- Sharma D, Murki S, Maram S, Pratap T, Kiran S, Venkateshwarlu V, Dinesh P, Kulkarni D, Kamineni B, T A, Singh G. Comparison of delivered distending pressures in the oropharynx in preterm infant on bubble CPAP and on three different nasal interfaces. Pediatr Pulmonol. 2020 Jul;55(7):1631-1639. PMID: 32237275.
- Devices and pressure sources for administration of nasal continuous positive airway pressure (NCPAP) in preterm neonates. Available from: https://www.cochrane.org/CD002977/NEONATAL_devices-and-pressure-sources-for-administration-of-nasal-continu-ous-positive-airway-pressure-ncpap-in-preterm-neonates
- Miller MJ, DiFiore JM, Strohl KP, Martin RJ. Effects of nasal CPAP on supraglottic and total pulmonary resistance in preterm infants. J Appl Physiol. 1985;68(1):141-146.
- Aly H, Mohamed MA. An experience with a bubble CPAP bundle: is chronic lung disease preventable? Pediatr Res. 2020 Sep;88(3):444-450. PMID: 31952073